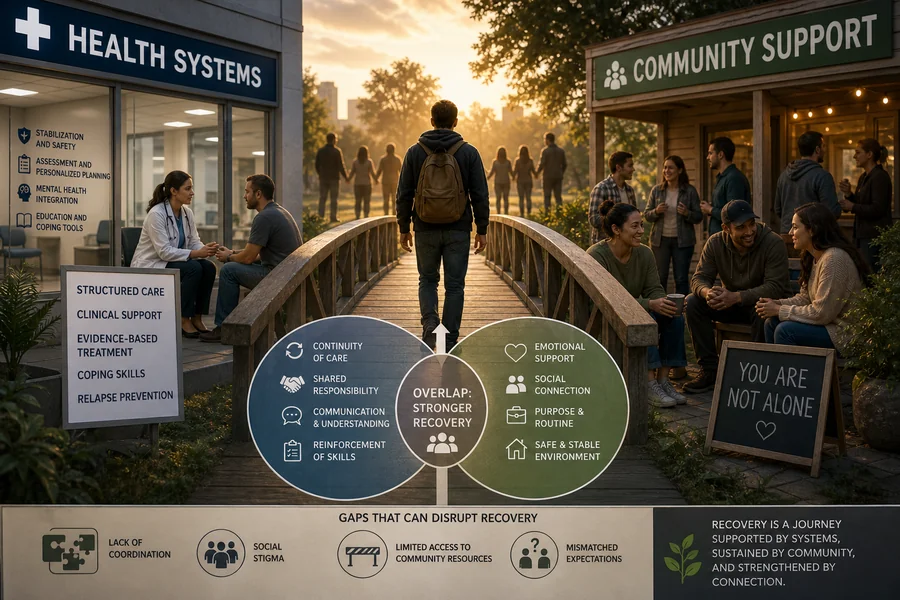
The Overlap Between Health Systems and Community Support in Early Recovery Stages
Early recovery from substance use is rarely a straight path. It tends to be shaped by a mix of structured care, personal readiness, and the everyday environments people return to after seeking help. In recent years, more attention has been given to how formal health systems and informal community support networks intersect—sometimes smoothly, sometimes with gaps that can affect long-term outcomes.
Understanding this overlap matters because recovery doesn’t exist in isolation. It is influenced by access to care, continuity of support, social connection, and the stability of a person’s surroundings. When these elements align, early recovery stages can feel more manageable and less overwhelming. When they don’t, the risk of setbacks often increases.
Early Recovery: A Sensitive Transition Phase
The early stages of recovery are often described as the most fragile period. This is when the body and mind are adjusting to the absence of substances, and when individuals are learning how to function without old coping mechanisms.
During this time, people may experience:
- Emotional instability or mood swings
- Sleep disruptions and fatigue
- Anxiety or uncertainty about the future
- Cravings or triggers tied to past routines
- Difficulty re-engaging with daily responsibilities
These challenges are not just medical—they are deeply personal and social. That’s where the overlap between health systems and community support becomes especially important.
Health systems may provide clinical stabilization and structured care, while communities offer the day-to-day environment where recovery is actually lived.
The Role of Health Systems in Early Recovery
Health systems typically represent the structured side of recovery support. This includes medical supervision, mental health services, counseling frameworks, and coordinated care plans designed to address both physical and psychological aspects of substance use.
In early recovery, health systems often focus on:
1. Stabilization and Safety
The initial priority is helping individuals reach physical and emotional stability. This includes managing withdrawal symptoms, monitoring health risks, and ensuring safety during a vulnerable transition period.
2. Assessment and Personalized Planning
Recovery is not one-size-fits-all. Health systems often assess physical health, mental health history, substance use patterns, and social conditions to create a more tailored approach.
3. Mental Health Integration
Many individuals entering recovery also experience co-occurring conditions like anxiety, depression, or trauma-related stress. Addressing these conditions early helps reduce relapse risk and improves long-term resilience.
4. Education and Coping Tools
Structured programs often introduce coping strategies for cravings, stress management techniques, and relapse prevention planning. These tools are meant to be carried beyond clinical settings into everyday life.
While these systems are essential, they cannot fully sustain recovery on their own. Once individuals step back into their communities, the environment plays a major role in whether progress continues or becomes harder to maintain.
Community Support as the Living Environment of Recovery
Community support refers to the informal, everyday structures that surround a person—family, peers, local networks, and social environments. Unlike clinical systems, these supports are ongoing and embedded in daily life.
Community support often includes:
1. Emotional Support Networks
Family members, friends, or peers in recovery can provide encouragement, accountability, and understanding during difficult moments. This emotional layer can significantly reduce feelings of isolation.
2. Social Reintegration
Returning to normal routines—work, school, or community activities—can be both grounding and challenging. Supportive environments help individuals rebuild identity and purpose beyond substance use.
3. Peer Connection
Shared experiences matter. Connecting with others who have gone through similar struggles often helps normalize the recovery process and reduces shame.
4. Environmental Stability
A stable living situation, safe neighborhoods, and reduced exposure to triggers all contribute to maintaining progress made during earlier stages of care.
Community support is not always structured or formal, but it is often what determines how sustainable recovery feels in the long run.
Where Health Systems and Community Support Overlap
The most effective recovery outcomes tend to occur when health systems and community support are not separate, but connected. This overlap creates continuity—meaning that progress made in structured care is reinforced rather than interrupted once a person returns to daily life.
1. Continuity of Care
One of the most important intersections is the transition from clinical support to everyday living. When care planning includes community integration from the beginning, individuals are less likely to feel abandoned after structured treatment ends.
2. Shared Responsibility
Recovery works best when responsibility is distributed. Health systems provide tools and guidance, while communities provide reinforcement and lived experience support.
3. Communication Between Systems and Families
When families or close support networks understand what recovery involves, they are better equipped to respond to challenges. Even simple awareness about triggers, stress responses, or emotional changes can make a significant difference.
4. Reinforcement of Coping Strategies
Skills learned in structured care—such as managing cravings or handling stress—become more effective when the surrounding environment supports their use.
Gaps That Can Disrupt Recovery
Despite growing awareness, there are still gaps between formal systems and community environments. These gaps can create friction in early recovery stages.
Lack of Coordination
When there is little communication between structured care and personal environments, individuals may feel unsupported or confused about next steps.
Social Stigma
Stigma remains one of the most persistent barriers. Negative perceptions around substance use can discourage individuals from seeking or maintaining support.
Limited Access to Community Resources
Not all communities have equal access to recovery-friendly environments, peer groups, or supportive networks.
Mismatched Expectations
Health systems may focus on structured progress, while communities may expect immediate behavioral change. This mismatch can create pressure during an already sensitive period.
The Importance of Social Environment in Recovery Stability
Research and lived experience both point to the same conclusion: environment matters. Even strong clinical progress can be disrupted if a person returns to an unstable or unsupportive setting.
Conversely, a supportive environment can strengthen recovery even when clinical support becomes less frequent over time.
This is why discussions around recovery increasingly include broader social factors such as housing stability, employment opportunities, and community inclusion.
For example, when people search for terms like Fresno Drug and Alcohol Detox, what they are often really seeking is not just short-term stabilization, but a pathway that connects medical care with long-term support systems that exist beyond the clinical setting.
Building Stronger Bridges Between Systems and Communities
Improving recovery outcomes requires more intentional connection between structured care and everyday environments. Some key approaches include:
1. Early Community Engagement
Involving family or support networks early in the recovery process helps reduce the shock of transition later on.
2. Education for Support Networks
When communities understand recovery as a process rather than a single event, they become more effective in supporting it.
3. Aftercare Integration
Recovery planning that includes follow-up support, peer groups, or community-based resources helps maintain continuity.
4. Reducing Stigma Through Awareness
Public understanding plays a major role in shaping how safe individuals feel returning to their communities.
Recovery as a Shared Ecosystem
Early recovery is not just a medical phase—it is a shared social experience shaped by both structured systems and human connection. Health systems provide stability, guidance, and clinical care, while communities provide continuity, belonging, and real-world reinforcement.
When these two areas overlap effectively, recovery becomes less about surviving a transition and more about building a sustainable way of living.
The challenge moving forward is not choosing between health systems or community support, but strengthening the bridge between them so that individuals are not left navigating early recovery alone.