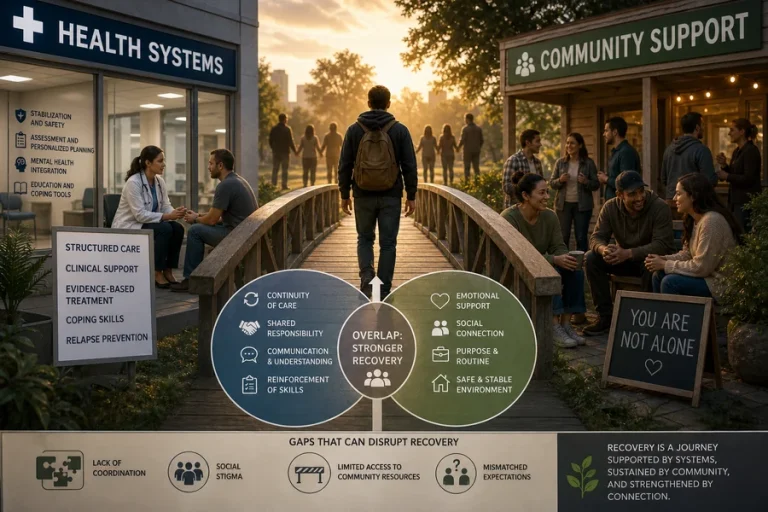
A Closer Look at Integrated Care Models in Addressing Substance Use and Mental Health Needs
For a long time, substance use and mental health challenges were often treated as separate issues, even when they clearly overlapped in a person’s life. Someone struggling with depression might also be coping with alcohol dependency. Another person dealing with anxiety might also be using substances as a way to manage stress. Yet the systems designed to help them were frequently divided, forcing individuals to move between providers, repeating their stories and often falling through the cracks.
In recent years, a shift has been taking place toward more connected, holistic approaches. Integrated care models are gaining attention because they acknowledge a simple but powerful truth: mental health and substance use are deeply interconnected, and treating one without the other often leaves gaps in recovery.
This article takes a closer look at how integrated care works, why it matters, and how it is reshaping support systems for individuals and families navigating complex behavioral health needs—including those seeking drug rehab in Massachusetts and similar settings where comprehensive care is becoming increasingly important.
Understanding Integrated Care in Behavioral Health
Integrated care refers to a coordinated system where mental health services, substance use treatment, and sometimes even primary healthcare are delivered together rather than separately. Instead of treating symptoms in isolation, providers work collaboratively to address the whole person.
At its core, integrated care is built on three ideas:
- Mental health and substance use conditions often occur together.
- Recovery is more effective when care is coordinated.
- A person’s physical, emotional, and social needs are all connected.
This model contrasts with traditional approaches where someone might see a therapist for depression, a separate counselor for addiction, and yet another provider for medical concerns. That fragmentation can create confusion, inconsistent treatment plans, and missed warning signs.
Integrated care tries to close those gaps.
Why Substance Use and Mental Health Are So Closely Linked
To understand why integrated care matters, it helps to look at the relationship between mental health and substance use.
Many people do not begin using substances in isolation. Often, there is an underlying emotional or psychological struggle involved. For example:
- Someone experiencing chronic anxiety may use alcohol to “calm down.”
- A person with unresolved trauma might use substances to numb emotional pain.
- Depression can lead to isolation, where substances become a coping mechanism.
Over time, substance use can also worsen mental health symptoms. What begins as temporary relief can develop into a cycle where both conditions reinforce each other.
This is why treating only one aspect—such as detoxing from substances without addressing anxiety or trauma—can make long-term recovery more difficult.
The Core Components of Integrated Care Models
Integrated care is not a single program but rather a framework that can take different forms. However, most models share several key components.
1. Collaborative Treatment Teams
Instead of working in isolation, professionals from different disciplines coordinate care. This may include counselors, therapists, medical providers, and social workers communicating regularly to align treatment goals.
2. Comprehensive Assessment
When a person enters care, their mental health, substance use history, physical health, and social circumstances are evaluated together. This helps avoid fragmented treatment plans.
3. Co-Occurring Disorder Treatment
Many individuals experience both mental health and substance use disorders at the same time. Integrated care specifically addresses these co-occurring conditions rather than treating them separately.
4. Continuity of Care
Recovery is not a short process. Integrated systems focus on long-term support, ensuring that individuals transition smoothly between levels of care without losing progress.
5. Personalized Recovery Plans
Instead of a one-size-fits-all approach, treatment is tailored to the individual’s specific needs, challenges, and strengths.
Why Traditional Approaches Often Fall Short
Historically, behavioral health care has been divided into “mental health treatment” and “addiction treatment.” While both are important, the separation can create real challenges.
Some of the most common issues include:
- Disconnected communication: Providers may not share information effectively.
- Conflicting treatment plans: One provider may focus on abstinence while another addresses underlying anxiety without coordination.
- Repeated storytelling: Individuals often have to retell their history multiple times, which can be emotionally exhausting.
- Gaps in care transitions: Moving from detox to therapy or outpatient care can feel abrupt and unsupported.
These gaps can increase the risk of relapse or disengagement from treatment altogether.
Integrated care aims to reduce these barriers by creating a more seamless experience.
The Role of Mental Health in Recovery
One of the most important shifts in modern care is the recognition that mental health is not a secondary concern—it is central to recovery.
Conditions like depression, PTSD, bipolar disorder, and anxiety disorders often influence substance use patterns. Without addressing these underlying issues, recovery can feel incomplete.
In integrated care models, therapy is not treated as optional or separate from addiction treatment. Instead, it becomes a core part of the recovery process. Evidence-based approaches such as cognitive behavioral therapy, trauma-informed care, and motivational interviewing are commonly used to support both emotional healing and behavioral change.
The Role of Physical Health in Integrated Care
Another important dimension of integrated care is physical health. Substance use often affects the body in significant ways, including sleep disruption, nutritional deficiencies, and chronic health conditions.
In integrated systems, medical professionals may be involved alongside behavioral health providers to ensure that physical health is not overlooked. This can include:
- Monitoring withdrawal symptoms
- Managing co-existing medical conditions
- Supporting sleep and nutrition recovery
- Addressing medication needs safely
By including physical health in the recovery process, individuals are more likely to experience sustainable improvement.
How Integrated Care Supports Long-Term Recovery
Recovery is not only about stopping substance use; it is about building a stable and meaningful life. Integrated care supports this by focusing on long-term stability rather than short-term fixes.
Some of the long-term benefits include:
Better Treatment Retention
When care feels coordinated and supportive, individuals are more likely to stay engaged in treatment.
Reduced Relapse Risk
Addressing mental health, triggers, and environmental stressors together helps reduce relapse risk.
Improved Emotional Regulation
Therapy and behavioral support help individuals develop healthier coping mechanisms.
Stronger Support Systems
Integrated care often involves family education and community resources, strengthening the support network around the individual.
The Human Side of Integrated Care
Beyond clinical definitions and treatment models, integrated care ultimately comes down to something more human: feeling understood.
Many individuals struggling with substance use and mental health challenges describe feeling fragmented—like their experiences are being split into pieces and examined separately. Integrated care brings those pieces together.
It acknowledges that a person is not just a diagnosis or a set of symptoms, but a whole individual shaped by experiences, relationships, and environment.
That shift in perspective can make a meaningful difference in how people experience care.
Growing Adoption in Modern Behavioral Health Systems
Across different regions, integrated care is becoming more widely adopted as awareness grows around co-occurring disorders. Treatment systems are increasingly moving toward collaboration between behavioral health, primary care, and community-based services.
In areas where access to coordinated services is expanding, such as in discussions around drug rehab in Massachusetts, integrated care models are often highlighted as a promising direction for improving outcomes and reducing long-term health disparities.
While implementation varies, the overall trend is clear: fragmented care is giving way to more connected systems.
Challenges in Implementing Integrated Care
Despite its benefits, integrated care is not without challenges.
Some common barriers include:
- Workforce shortages in behavioral health fields
- Limited coordination between systems
- Insurance and funding constraints
- Differences in training among providers
- Structural separation between mental health and addiction services
These challenges mean that integration is an ongoing process rather than an immediate solution. However, progress continues as systems recognize the importance of coordination.
Looking Ahead: The Future of Integrated Care
The future of behavioral health care is likely to become even more integrated, with increased use of collaborative models and technology-supported coordination.
Some emerging trends include:
- Greater use of shared electronic health records
- Expansion of community-based care teams
- Increased focus on trauma-informed approaches
- Stronger integration of social services, such as housing and employment support
These developments reflect a growing understanding that recovery is influenced by far more than clinical treatment alone.
Final Thoughts
Integrated care represents a significant shift in how substance use and mental health challenges are understood and addressed. By moving away from fragmented systems and toward coordinated, person-centered care, it offers a more complete and realistic approach to recovery.
While challenges remain in implementation, the direction is clear: treating the whole person, not just isolated symptoms, leads to better outcomes.
For individuals and families navigating complex behavioral health needs, this approach offers something essential—continuity, connection, and a more compassionate path forward.